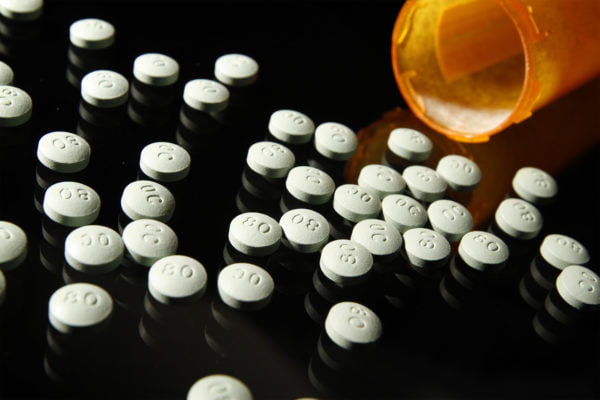
According to the CDC, opioid prescriptions are on the decline.
The number of prescriptions for opioids written by health care providers declined between 2012 and 2015, the government reported Thursday, introducing a glimmer of progress in efforts to quell the worst drug epidemic in U.S. history.
The Centers for Disease Control and Prevention said prescriptions for highly addictive painkillers such as oxycodone dropped 13.1 percent over the three-year period, from 81.2 per 100 people to 70.6.
[Opioids hospitalize nearly 23 Mainers a day]
But Anne Schuchat, the CDC’s acting director, expressed tempered optimism about the first national decline in opioid prescriptions that the CDC has reported since the crisis began in the late 1990s. She said the prescription rate is still triple the level it was in 1999 and four times as much as it is in some European countries. Even at the reduced prescribing rate, she said, enough opioids were ordered in 2015 to keep every American medicated round-the-clock for three weeks.
“It looks a little bit better, but you really have to put that in context,” Schuchat said in an interview. “We’re still seeing too many people get too much for too long.”
The overprescribing of legal opioids sparked the addiction crisis, but some addicts eventually move to cheaper or stronger drugs, especially if they run into difficulty obtaining prescription opioids. In recent years the overdose death rate from illicit drugs, such as heroin and fentanyl, has risen much faster than the rate of overdoses from medical narcotics. That means the decline in prescriptions may trigger fewer first-time addictions in the future, Schuchat said.
The improvement should be viewed “as prevention,” she said. “The fewer we get started, the fewer we get addicted to opioids.”
[The Penobscot County Jail is trying something new to fight the opioid crisis]
Gary Mendell, founder of the anti-drug advocacy group Shatterproof, noted “the improvements being made,” citing estimates that 80 percent of opioid abusers first become addicted to prescription narcotics, not street drugs. But, he said, the reduction is “not even close to what could occur in this country.”
In particular, Mendell said, prescribing practices should be measured and responded to in real time. The cumbersome CDC process of collecting data from states and counties is inefficient, he said.
“Can you imagine being on a conference call with a company and they announce data that’s two years old?” said Mendell, a former hotel executive. “There’s a simple saying in business: What doesn’t get measured doesn’t get done.”
The opioid crisis appears to have left no community untouched as it’s mushroomed into an epidemic since the turn of the century. Prescription opioids alone killed nearly 180,000 people from 2000 to 2015 and those overdoses, abuse and dependence on medical narcotics created an annual “economic burden” estimated at $78.5 billion, according to the new report.
In 2015, the latest year for which the CDC has released data, more than 33,000 people died of overdoses that involved an opioid, including more than 15,000 who had taken a prescription narcotic. Nearly 13,000 more were killed by overdoses of heroin.
State data and a nationwide survey conducted by the New York Times indicate that those figures may be rising sharply in 2016.
More than two million people are addicted to opioids, the government estimates. In 2014 alone, there were 1.27 million emergency room visits or inpatient hospital stays for opioid-related health problems, another government agency reported in June.
The critical shortage of treatment for people with opioid use disorder also has complicated plans by the President Trump and Republicans in Congress to repeal and replace the Affordable Care Act. States confronting major drug problems have resisted federal proposals to roll back Obamacare’s expansion of Medicaid, which is helping to fund treatment for many people.
[Maine’s health care providers have a chance to save lives lost to opioids. It’s time they seize it.]
There are also indications that prescriptions for opioids have been dropping since 2015. In the past year, some private-sector data collectors have reported prescription declines on par with the data in the CDC report. Customers of Cigna Health Insurance, for instance, have consumed nearly 12 percent fewer opioids in the past year, according to Will Lopez, senior medical director of Cigna Behavioral Health.
The CDC report also confirmed another critical factor in the crisis: It found wide disparities in opioid prescriptions in counties across the nation. Doctors in some counties in hard-hit parts of Appalachia, the southwest and New England prescribed the equivalent of 958 to 5,543 milligrams of morphine per capita in 2015. In other locations, prescribers authorized zero to 454 milligrams in the same year.
The report also determined, as other researchers have, that opioids are more heavily prescribed in small town America, in counties with larger white populations, and in places where unemployment and Medicaid enrollment are higher. It also found that they are prescribed more frequently in counties where arthritis and diabetes rates are higher than average.
Still, those factors only explain about a third of the variation among counties, Schuchat said. “That suggests to me that clinicians may not know what the right amount of prescribing is. They may be prescribing based on custom and tradition and what they were taught” in medical school, she said.
In the last few years, medical and public health authorities, including the CDC, have been urging doctors to cut back on the number of pills, the dose and the duration of the prescriptions they offer – a turnaround from just 15 years ago, when a nationwide movement urged physicians to more aggressively treat their patients’ pain. Even before the CDC issued guidelines last year, studies were warning prescribers of the dangers of dispensing too many opioids.
The data indicate that at least some prescribers are heeding the message. Nationally, prescribing peaked at the equivalent of 782 milligrams of morphine per person in 2010, declining to 640 milligrams per person in 2015.
The study also found a continued increase in long-term prescribing of opioids. The average length of prescriptions rose steadily from about 13 in 2006 to about 18 in 2015, the data show. But Schuchat cautioned that as fewer people are receiving short-term prescriptions, those who take opioids for years for chronic pain may have skewed the average. The CDC has said that there is no evidence that opioids are effective long-term and suggests that people with chronic pain, one of the most common reasons for visiting a health-care provider, seek alternatives.
“Improving the management of chronic pain is very important,” Schuchat said. “There are multiple approaches. Larger-scale studies suggest that opioids, even high-dose opioids, are not in the long run effective for chronic pain, and in the long run may even be dangerous.”
[“Source-bangordailynews”]